INTRODUCTION
During the restorative process for an indirect restoration, it is common to use provisional restorations in order to avoid sensitivity, infection, and tooth movement. It is the last step at the end of the preparation appointment, and an adverse outcome at this stage could mean an emergency visit to your office or a problematic appointment during the placement of the final prosthesis. The temporary cement used should provide adequate strength to retain the restoration during function; however, the retention developed by the provisional cement should be low enough to allow removal of the provisional restoration without causing damage or alteration to the prepared surface before the definitive restoration is placed.1
Some clinical situations may dictate the need for long-term provisional restorations,2,3 and in these cases, using a luting agent with good mechanical properties, low solubility, and good adhesion is critical to avoid problems with cement washout, marginal leakage, bacterial infiltration, and caries.3
According to Farah and Powers,4 an ideal temporary cement should exhibit the following characteristics: easy removal of excess cement from around the margins; good marginal seal to help minimize sensitivity; good retention but easy removal of the temporary prosthesis; low solubility in oral fluids; and compatibility with provisional resin restorations, resin core materials, bonding agents, and permanent cements.
Several factors influence the retention of the provisional restoration, including the convergence of the preparation, preparation height,5-8 and cement.9 The ADA Professional Product Review (2011)10 presents a list of criteria to consider when selecting provisional cements, such as:
- Type of clinical application
- Appropriate working and setting time
- Degree of adhesion to dentin and enamel
- Ease of mixing and dispensing
- Ease of application and removal after setting
- Biocompatibility with other restoratives, pulp, and soft tissues
- Sensitivity to moisture during and after setting
- Viscosity for handling and application
- Solubility
- Erosion
- Strength
- Toughness
- Stiffness (elastic modulus).
Besides the criteria listed above, there is a need to evaluate the composition of temporary cements in order to select the best candidate for each clinical case. Different compositions of provisional cements are commercially available, including polycarboxylate, zinc oxide eugenol (ZOE), zinc oxide noneugenol (ZONE), and resin-based cements.4
Types of Temporary Cements
Polycarboxylate temporary luting cements present low postoperative sensitivity, adequate retention, and easy cleanup. Examples of this category are: Cling2 (CLINICIAN’S CHOICE) and Hy-Bond (Shofu Dental).
ZOE temporary luting cements are commonly used because of their sedative effect on sensitive teeth.11 It is well documented that eugenol is able to penetrate and diffuse throughout the dentin12,13 and can affect the bond strengths provided by resin materials used for definitive restorations.14,15 It presents an excellent antibacterial effect.4 Examples of this category are: RelyX Temp E (3M ESPE), Temp-Bond (Kerr), Flow Temp (Premier Dental Products), SensiTemp ZOE (Sultan Healthcare), and Hy-Bond ZOE (Shofu Dental).
ZONE temporary luting cements are designed to replace eugenol with various types of carboxylic acids16 that do not interfere with definitive cementation.17 They have the characteristics of being compatible with resin provisional materials, are compatible with permanent resin cements, and show greater retention compared to ZOE cements18 but have no sedative effect on the pulp. Examples of this category are RelyX Temp NE (3M ESPE); Temp-Bond NE (Kerr); Freegenol, Nogenol, and Temp Advantage (GC America); NexTemp (Premier Dental Products); SensiTemp (Sultan Healthcare); PowerTemp (J. Morita USA); Provicol (VOCO America); Systemp.cem (Ivoclar Vivadent); UltraTemp (Ultradent Products); and Proviscell (Septodont).
Resin temporary luting cements present high strength, excellent retention, better aesthetics, and easy cleanup. However, these temporary cements have a higher incidence of microleakage, discoloration, and odor associated with their use. Examples of temporary resin luting cements are: Systemp.link (Ivoclar Vivadent), Temp-Bond Clear (Kerr), ImProv (Nobel Biocare), Premier Implant Cement (Premier Dental Products), and SensiTemp Resin (Sultan Healthcare).
It should be noted (as it also relates to the eugenol-containing temporary cements discussed earlier) that Woody and Davis19 have suggested that poor dentin bond strength after temporary cementation may result from the presence of cement remnants and not from just the eugenol. These remnants have been observed microscopically on macroscopically clean surfaces.20,21 Because of this, it is important to use a cement that cleans easily and does not leave remnants on the surface of the tooth. Of all the temporary cement categories, polycarboxylate cements are the easiest to clean.4
Questions to Ask When Making a Selection
Finally, when selecting a temporary cement, the clinician should pose and answer some critical questions:
- How long is the provisional to remain in place?
The temporary cement should be able to restore the marginal integrity and resist dissolution in oral fluids. The longer the time the provisional restoration will be in place, the lesser should be the solubility of the temporary cement in order to maintain the proper seal at the margins. A cement suitable for a one- or 2-week cementation will not be suitable for a longer period of time such as is required after periodontal surgery. - How retentive is the preparation?
Short or convergent crown preparations or onlay preparations present less retentive walls requiring a more retentive temporary cement; however, preparations that demonstrate good retentive features demand a weaker cement. Assessing the number and draw of each preparation will allow you to select the cement with the right amount of retention but still allow for easy removal. - Is an adhesive technique to be used for cementation of the permanent restoration?
It is demonstrated in the literature that eugenol permeates the tooth structure and disrupts the bond of the dental adhesive and cement. So the selection of the right temporary cement demands an understanding of the clinical situation, the type of permanent restoration selected, the oral environment, and temporary cement properties. - Is the clinician working in an aesthetic zone?
In some cases on the anterior dentition, the temporary cement may discolor the interim restoration if the provisional is too thin. In general, the tooth reduction required for a PFM or all-ceramic crown will provide sufficient thickness for the provisional restoration and the cement will not affect the shade. Thin preparations like veneers may allow show-through of the temporary cement. In such a situation, a clear cement should be used to avoid discoloration. Keep in mind that function, when possible, should supersede aesthetics for this phase of treatment.
CASE REPORT
Diagnosis and Treatment Planning
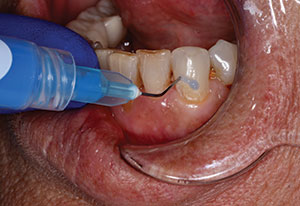
A 55-year-old male patient presented with the chief complaint of “a small piece of my tooth fell off and I would like to restore it.” Intraoral and radiographic examinations were done and it was noted that the tooth in question (No. 5) was heavily restored (Figure 1). It presented with a large MODL resin composite restoration, plus a sizable amalgam restoration on the lingual surface margins extending 2.0 mm subgingivally. The resin composite restoration also demonstrated signs of leakage at the margins (Figure 2) as well as a fracture at the lingual cusp. It was also noted that tooth No. 6 had a large defective resin composite restoration.
 |
 |
| Figure 1. Lingual view of tooth No. 5 with a large MODL resin composite restoration plus a large amalgam restoration. Note large restoration at the distal of tooth No. 6. | Figure 2. Labial view of tooth No. 5 with resin composite restoration extending from mesial and distal surfaces to almost the center of buccal surface. Note signs of leakage at the margins. |
After discussing the treatment options with the patient, the decision was made to proceed by placing a crown on tooth No. 5, and to restore tooth No. 6 using composite resin.
Clinical Protocol
Prior to tooth reduction, an impression using a disposable metal tray (TempTray [CLINICIAN’S CHOICE]) loaded with vinyl polysiloxane (VPS) matrix material (Template [CLINICIAN’S CHOICE]) (with a setting time of 30 seconds) was taken to facilitate the fabrication of the provisional restoration after the crown preparation (Figure 3). An extra large mixing tip (7.5 mm) was used to easily and efficiently dispense the VPS material into the tray; the extra large tip allowed the proper positioning of the tray to be done quickly before the material started to set.
After the initial crown preparation and removal of amalgam, it was noted that the remaining tooth structure was deemed insufficient to properly retain a permanent indirect restoration. Before the fabrication of the provisional restoration, the large undercut left by the amalgam was blocked with a glass ionomer (GC Fuji Plus [GC America]) (Figure 4) and the margins were refined to allow proper adaptation of the provisional restoration (Figure 5). Once the preparation was completed and after re-assessment of the remaining tooth structure, the decision was made to refer the patient for root canal therapy (RCT) and for crown lengthening to correct the biological width that was affected by the old restorative procedure.
 |
 |
| Figure 3. Disposable metal tray loaded with VPS matrix (impression) material (Template [CLINICIAN’S CHOICE]). | Figure 4. Tooth reduction for an all-ceramic crown. Undercuts were blocked out with a glass ionomer (GC Fuji Plus [GC America]). |
At this stage of treatment, using the matrix fabricated earlier, a provisional restoration was fabricated using a bis-acryl material (Temptation [CLINICIAN’S CHOICE]) to protect the tooth during the subsequent phases of treatment. The bis-acryl material was placed into the impression and a small quantity of Temptation was also applied around the margins of the preparation in order to reduce/eliminate voids. After polymerization, the provisional material was removed from the matrix and trimmed. The margins were inspected, the occlusion was adjusted, and the provisional was coated with an unfilled light-cure resin (Glisten [CLINICIAN’S CHOICE]) in order to provide a high gloss shine finish. This technique, using an unfilled resin, reduces the time used to polish provisional restorations and assists in the removal of the temporary cement due to the smooth surface obtained. Surface roughness, which is a common patient complaint with bis-acryl temporaries, is eliminated with the glaze, and the wear of the temporary restoration is reduced as well.
After asking the 4 questions listed above, we decided to use a temporary cement that presents low solubility, easy cleaning (since it needs to protect the tooth for a moderate period of time), good retention but easy removal, and would not interfere with permanent cementation. The selection of a polycarboxylate (resin-reinforced) cement was made due to the depth of the preparation and the need for the reduction for the inflammatory response at the gingival margins prior to periodontal surgery. The thickness of the provisional restoration was sufficient enough to not have its color changed by the temporary cement (Cling2) selected for this case (Figures 6 to 8).
 |
 |
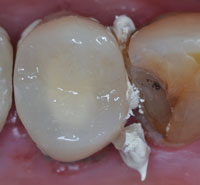
| Figure 5. Occlusal view of the initial preparation of tooth No. 5. Note the smoothness of the margins obtained with a fine diamond bur (Edge [CLINICIAN’S CHOICE]). Note also the inflammation present in the gingival tissues due to invasion of the biological width by the old restorations. | Figure 6. A bis-acryl provisional restoration cemented with Cling2 (CLINICIAN’S CHOICE) showing excess of cement as prescribed by the manufacturer. |
 |
 |
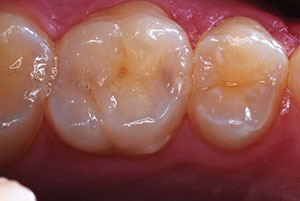
| Figure 7. After curing, the excess temporary cement was easily removed. | Figure 8. Occlusal view of the restoration after cleaning the cement. Note the glossy appearance of the temporary restoration coated with an unfilled resin (Glisten [CLINICIAN’S CHOICE]). |
One week after tooth preparation, the patient was asymptomatic, and it was decided that the periodontal surgery should be done first, in order to provide the proper isolation during the next restorative phase that included a Class III and V (No. 6) and RCT (No. 5). The provisional was removed (Figure 9) and an improvement in the health of gingival tissue was noted. Periodontal surgery (crown lengthening) was done with osteotomy in order to re-establish the biological width, leaving the margins of the preparation at a distance of 3 mm from the bone crest all around the tooth (Figure 10). The old resin composite restoration fell off during the procedure and a temporary restoration was placed until the following appointment. A couple of non-absorbable, wax-coated braided silk sutures (3-0 Sofsilk [Tyco Healthcare Group]) were placed and the surgical site protected with a periodontal dressing (Coe-Pack [GC America]).
One week after surgery, the sutures and periodontal dressing were removed. The first quadrant was isolated with a rubber dam and the temporary restoration of tooth No. 5 was removed. After the final preparation for a Class III restoration, the tooth was etched with a 35% phosphoric acid (Ultra-Etch [Ultradent Products]), rinsed, and dried. The dentin was rehydrated with a glutaraldehyde-based desensitizer (G5 [CLINICIAN’S CHOICE]) and a layer of bonding agent was applied and light-cured (MPA [CLINICIAN’S CHOICE]). A radiopaque flowable hybrid liner (De-Mark [Cosmedent]) was placed as shown on this picture and light-cured prior to the restoration (Figure 11). The Class III restoration was finished with a nanofilled hybrid composite resin (Renamel Nano [Cosmedent]). After occlusal adjustments, the restoration was finished and polished (Top Finisher System [Cosmedent]) (Figure 12). The healing site was protected again with Coe-Pack for another 7-day period. This second application of the periodontal dressing helps with the guidance of the tissue healing.
 |
 |
| Figure 9. One week after the crown preparation, the provisional was removed, and the improvement in healing of the gingival tissue around the preparation is notable. | Figure 10. Periodontal surgery was performed and the biological widths were restored. A couple of sutures (3-0 Sofsilk [Tyco Healthcare Group LP]) and a periodontal dressing (Coe-Pack [GC America]) were placed to protect the surgical site. |
 |
 |
| Figure 11. Placement of a radiopaque flowable hybrid liner (De-Mark [Cosmedent]) after etching and bonding, prior to the restoration. | Figure 12. The Class III composite resin restoration (Renamel Nano [Cosmedent]). |
 |
| Figure 13. View of the surgical site at 4 weeks postoperatively. Note positioning of the gingival tissue around the provisional restoration with the margins of preparation located at supragingival level. |
Four weeks after the initial treatment, the gingival tissue around the provisional restoration was re-evaluated (Figure 13) and the patient was referred for RCT and would later receive a fiber post (Macro-Lock [RTD-CLINICIAN’S CHOICE]) with a core build-up material (Zircules [CLINICIAN’S CHOICE]), followed by an all-ceramic crown.
CLOSING COMMENTS
In a crown and bridge treatment, every step is an opportunity for success or failure—for instance, a poorly-fabricated provisional restoration with nondefined margins will lead to tissue inflammation, in turn complicating the next step of treatment (impression or cementation); whereas a well-fabricated provisional with inconspicuous margins will ensure healthy surrounding tissues (gingiva), which will facilitate better impressions or cementation. It is also important to highlight that the careful selection of a temporary cement is as important as the fabrication of the provisional restoration, since the cement must retain the provisional during function, seal the margins, and reduce postoperative sensitivity.
Acknowledgment
The author would like to acknowledge the educational grant and materials received from Clinical Research Dental/CLINICIAN’S CHOICE used to support this article.
References
- Ramp MH, Dixon DL, Ramp LC, et al. Tensile bond strengths of provisional luting agents used with an implant system. J Prosthet Dent. 1999;81:510-514.
- Rosenstiel SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 2nd ed. St Louis, MO: Mosby; 1995:353.
- Baldissara P, Comin G, Martone F, et al. Comparative study of the marginal microleakage of six cements in fixed provisional crowns. J Prosthet Dent. 1998;80:417-422.
- Farah JW, Powers JM. Temporary cements. The Dental Advisor. 2005;22(6):2-4.
- el-Mowafy OM, Fenton AH, Forrester N, et al. Retention of metal ceramic crowns cemented with resin cements: effects of preparation taper and height. J Prosthet Dent. 1996;76:524-529.
- Bresciano M, Schierano G, Manzella C, et al. Retention of luting agents on implant abutments of different height and taper. Clin Oral Implants Res. 2005;16:594-598.
- Bernal G, Okamura M, Muñoz CA. The effects of abutment taper, length and cement type on resistance to dislodgement of cement-retained, implant-supported restorations. J Prosthodont. 2003;12:111-115.
- Jørgensen KD. The relationship between retention and convergence angle in cemented veneer crowns. Acta Odontal Scand. 1955;13:35-40.
- Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: A review of the current literature. J Prosthet Dent. 1998;80:280-301.
- ADA Professional Product Review. Temporary Cements. 2011;6(1):13-16.
- Abo-Hamar SE, Federlin M, Hiller KA, et al. Effect of temporary cements on the bond strength of ceramic luted to dentin. Dent Mater. 2005;21:794-803.
- Camps J, About I, Gouirand S, et al. Dentin permeability and eugenol diffusion after full crown preparation. Am J Dent. 2003;16:112-116.
- Kielbassa AM, Attin T, Hellwig E. Diffusion behavior of eugenol from zinc oxide-eugenol mixtures through human and bovine dentin in vitro. Oper Dent. 1997;22:15-20.
- Olin PS, Rudney JD, Hill EM. Retentive strength of six temporary dental cements. Quintessence Int. 1990;21:197-200.
- Paige H, Hirsch SM, Gelb MN. Effects of temporary cements on crown-to-composite resin core bond strength. J Prosthet Dent. 1986;55:49-52.
- Anusavice KJ. Phillips’ Science of Dental Materials. 11th ed. St. Louis, MO: Saunders; 2003:492.
- Bayindir F, Akyil MS, Bayindir YZ. Effect of eugenol and non-eugenol containing temporary cement on permanent cement retention and microhardness of cured composite resin. Dent Mater J. 2003;22:592-599.
- Dilts WE, Miller RC, Miranda FJ, et al. Effect of zinc oxide-eugenol on shear bond strengths of selected core/cement combinations. J Prosthet Dent. 1986;55:206-208.
- Woody TL, Davis RD. The effect of eugenol-containing and eugenol-free temporary cements on microleakage in resin bonded restorations. Oper Dent. 1992;17:175-180.
- Terata R, Nakashima K, Obara M, et al. Characterization of enamel and dentin surfaces after removal of temporary cement—effect of temporary cement on tensile bond strength of resin luting cement. Dent Mater J. 1994;13:148-154.
- Watanabe EK, Yatani H, Ishikawa K, et al. Pilot study of conditioner/primer effects on resin-dentin bonding after provisional cement contamination using SEM, energy dispersive x-ray spectroscopy, and bond strength evaluation measures. J Prosthet Dent. 2000;83:349-355.
Dr. Gildo Santos received his DDS (1986) and MSc in dental clinics (1999) from Federal University of Bahia, and PhD in prosthodontics (2003) from University of São Paulo. He was appointed as assistant professor, Division of Restorative Dentistry at the University of Western Ontario Schulich School of Medicine and Dentistry in 2006 and in 2011 was appointed chair of the Division of Restorative Dentistry. Dr. Santos joined the Faculty of Dentistry as an associate professor at the Federal University of Bahia (Brazil) and served from 1992 to 2006. He maintains an active prosthodontic practice, is coordinator of the CAD/CAM program along with other administrative roles and scholarly activities. He has several publications in international journals and has trained and mentored graduate students in the area of biomaterials research throughout his career. Dr. Santos is also a consultant to the dental industry. He can be reached via e-mail at gildo.santos@schulich.uwo.ca.
Disclosure: Dr. Gildo Santos is a paid consultant for Research and Development for Clinical Research Dental and CLINICIAN’S CHOICE.
Dr. Maria Jacinta Santos received her DDS (1988) and MSc in dental clinics (1999) from Federal University of Bahia, and PhD in operative dentistry (2003) from University of São Paulo. She was appointed as assistant professor, Division of Restorative Dentistry at the University of Western Ontario Schulich School of Medicine and Dentistry in 2009. She joined the Faculty of Dentistry as an associate professor at the Federal University of Bahia (Brazil) and served from 1993 to 2006. Mentoring graduate students in their biomaterials research studies at various stages of her career, she has also had a number of scientific articles published in leading international journals. She can be reached via e-mail at jacinta.santos@schulich.uwo.ca.
Disclosure: Dr. Maria Santos reports no disclosures.