INTRODUCTION
Let’s face it, placing successful posterior composites is exacting, tedious, and time consuming. The process includes achieving the necessary isolation, selecting and placing an appropriate matrix, precise execution of the adhesive steps, the placement of a flowable resin or resin ionomer liner and finally, the incremental placement, adaptation, and light curing of at least 2 or more layers of composite. Add to this sculpting, adjusting the occlusion, and finishing and polishing; and you have a procedure that just takes too much time. This in turn can produce a profitability problem for dentists who have contracts with insurance companies. In a recent article,1 Tom Limoli Jr stated that the average fee accepted by insurance companies in the United States for a Class II composite is $195 (range $137 to $241). Given today’s overhead per hour, dentists need material and technology advancements so that posterior composites can be placed faster, easier, and profitably without taking compromising shortcuts.
In recent years, materials have been introduced in an attempt to reduce some of the time and effort needed for layering and adaptation when placing posterior composites. One such composite resin material, Quixx (DENTSPLY Caulk) is advocated as a true “bulk fill” composite. Nevertheless, because of its high viscosity, it still might be prudent to place a low viscosity composite resin or low viscosity resin ionomer liner to achieve intimate adaptation to the pulpal and gingival floors. Although one 4-year clinical study2 showed an acceptable annual failure rate of 2.7% (a literature review analysis of posterior composite restorations reports annual failure rates for Class II composites range from 0% to 7% with a mean of 2.2%3), a real drawback of a restoration using this material is its translucency. The high translucency allows for a 4 mm depth of cure in 10 seconds using a light with a minimum of 800 mW/cm2 (manufacturer’s directions for use). Unfortunately, this necessary translucency can cause restorations to look gray (low value) in appearance. (Note: The author uses the term “bulk fill” to mean the entire cavity is filled in one single increment. Recently, some manufacturers are using this term in their advertisements to describe their composite material if it cures up to 4 mm. This is whether or not that amount can, or should, be used to fill a cavity in one increment.)
Calset (AdDent) is a technology for delivering a heated high viscosity composite and has been in the marketplace for some time. This technology heats the composite resin to 60°C, which lowers the viscosity, allowing the material to readily adapt to the cavity walls. In addition, theoretically, a heated composite should cure more easily (ie, require less light curing time) and reach a higher conversion ratio. This, in turn, should increase physical properties. In vitro data seems to confirm these claims;4,5 however, a recent in vivo study found minimal increase in conversion (3% to 4%) and concluded that reducing the light curing time is not recommended.6 The data showed that the tooth acts as a heat sink. Therefore, by the time the composite is removed from the heating unit, adapted to the cavity and light-cured, the material has quickly cooled to just slightly above tooth temperature. Whereas using this technology may preclude using a low viscosity liner, the restorative composite, depending on shrinkage and depth of cure, would still require layering for average-sized cavities.
More recently, a low viscosity composite, Surefil SDR (DENTSPLY Caulk) has been introduced. It is promoted as a flowable with a reported high depth of cure (4.1 mm) allowing placement of a large incremental base. This base is then surfaced with a high viscosity restorative composite resin. With a polymerization shrinkage of 3%,7 Surefil SDR would not be classified as a low shrink (< 2%). However, the manufacturer claims low shrinkage stress which is actually more significant.8 The appeal of this material is that, for the majority of cavities, a well adapted posterior composite restoration with good aesthetics can be achieved in less time because only 2 layers of composite are placed and cured; and only the second layer needs adaptation and sculpting.
New Materials and Technology
 |
 |
| Figure 1. SonicFill (Kerr). | Figure 2. When the handpiece is activated, liquefaction occurs, and the composite is rapidly extruded to fill the cavity. Upon deactivation, Sonicfill begins to return to a high-viscosity state. |
A new composite resin that is placed with the assistance of a sonic handpiece has recently been introduced. This material (SonicFill [Kerr]) (Figure 1) and technology increases the ease and efficiency of posterior composite placement even further. In essence, this composite resin is capable of delivering an aesthetic composite restoration in one true “bulk fill” increment. It is a high viscosity restorative composite which comes in tooth-colored shades (A1, A2, A3) and opacity, yet has a high depth of cure (5 mm). The customized composite is provided in a unidose tip. It is inserted into the cavity using a uniquely designed sonic handpiece. The handpiece fits KaVo MULTIflex air connections, as well as other brands, when using a compatible adaptor available from several manufacturers, including Kerr. When the tip is placed into the cavity and the handpiece activated, liquefaction occurs, resulting in an 87% drop in viscosity. The cavity fills in seconds. When the activation is ceased, the material begins returning to a high viscosity to allow for sculpting (Figure 2). When in the activated state, the composite material does not appear to reach what would be called a “flowable” state. However, the liquefaction achieved, along with the sonic vibration, yields optimal cavity adaptation in the same manner as a true flowable. Independent testing has shown SonicFill to have a 5-mm depth of cure with a bottom to top Rockwell hardness ratio of 80% or better.9,10 The high depth of cure is not accomplished by raising the translucency of the material, therefore the final aesthetics of the restoration ranges from good to very good. In the author’s experience, the majority of posterior cavities measure 5 mm or less; this means most posterior composite resin restorations can be restored quickly and efficiently in a single, rapidly placed true “bulk fill” increment without the need for a liner. Of course, for cavities greater than 5 mm, the first increment is pressed to place and cured before a second increment is placed. It should be noted, that although the bottom to top depth of cure ratio is above 80% for a 10-second cure using a light with an output greater than 1,000 mW/cm2, the manufacturer recommends additional time to account for the distance between the material and the light tip when curing (see Kerr’s directions for use because of variations in power output among different curing lights). Finally, SonicFill has been shown to have similar or better mechanical properties when compared to other restorative composite resins in the marketplace.9,10
CAS
E REPORT
The Technique
 |
 |
| Figure 3. An amalgam filling with poor contact and recurrent caries. | Figure 4. The amalgam, any base or liner, and all caries are removed. |
 |
 |
| Figure 5. A matrix and wedge (Triodent) were placed and the contact area was burnished. | Figure 6. The maximum cavity depth from the gingival floor to the adjacent tooth marginal ridge is measured using a periodontal probe. |
 |
 |
| Figure 7. The adhesive was placed and light-cured. |
Figure 8. The unidose tip was placed in contact with the deepest part of the cavity. |
 |
 |
| Figure 9. To reach the base of cavities, the opening diameter of the tips (SonicFill Unidose tips [Kerr]) (1.1 mm) are smaller than typical composite unidose tips. | Figure 10. Upon handpiece activation, the viscosity of the composite drops and it is rapidly extruded, filling the cavity in seconds. The tip was kept in the material and withdrawn as the cavity filled. |
 |
 |
| Figure 11. The filled cavity. | Figure 12. Using an instrument with a Teflon tip (Comporoller [Kerr]), the material was pressed down and wiped away at the margins. |
A patient presented with a leaking amalgam in a lower premolar requiring replacement (Figure 3). After local anesthesia and placement of the rubber dam (Hygenic Rubber Dam, [Coltène Whaledent]) the existing amalgam, liner/base and recurrent caries were removed (Figure 4). A sectional matrix and wedge (Triodent) were placed, and the contact area was burnished (Figure 5). The cavity measured less than 5 mm from the gingival floor to the marginal ridge of the adjacent tooth (Figure 6). After etching the enamel and dentin with a 30% to 40% phosphoric acid, a dentin/enamel adhesive (Optibond FL [Kerr]) was placed and light-cured according to the manufacturer’s directions (Figure 7). The SonicFill tip was placed into the bottom of the proximal box (Figure 8). The 1.5-mm opening diameter of the tip’s cannula allows access to small cavities (Figure 9). When the handpiece was activated, the cavity filled in less than 4 seconds (Figures 10 and 11). (The handpiece is slowly withdrawn as the cavity fills, with the tip staying within the material.) A round-ended condenser or a silicone-tipped instrument (Comporoller [Kerr]) was used to press down on the material and simultaneously wipe away excess at the margins (Figure 12). This composite resin material is nonsticky and does not slump, allowing for quick and easy shaping/sculpting with a bladed instrument (Figures 13 and 14). Upon completion, the restoration was light-cured from the occlusal for 20 seconds with a curing light providing high output. In this case, the Demi Plus LED (Kerr) was used. After removing the wedge and matrix, the restoration was light-cured again for 20 seconds from the buccal and the lingual aspects (Figures 15 and 16). Any excess adhesive and composite on the buccal or lingual was easily removed with a No. 12 blade in a scalpel handle (Figure 17). The rubber dam was then removed and the occlusion adjusted. It is the author’s preferred technique to retain any bonded occlusal flash and merely feather it with a carbide finishing bur 7404 (Axis Dental) (Figure 18). Final finishing and polishing were accomplished quickly with a one-step rubber instrument (Progloss [Axis Dental]), and wetted with water (Figure 19). This composite resin’s finish will be retained, reducing the chance for staining over time. When dried, SonicFill will be seen to have a very smooth matte finish, which does not pick up stain. Whereas a retained high gloss finish is important for anterior restorations, posterior restorations are always viewed wet by patients (Figure 20).
A second case is illustrated in photos (Figures 21 and 22), showing 2 SonicFill restorations in molars at 10 months post-op.
 |
 |
| Figures 13 and 14. The nonsticky, nonslumping material was rapidly sculpted using the tooth inclines as a guide. |
 |
 |
| Figures 15 and 16. After light curing from the occlusal, the matrix assembly was removed and additional light-curing was done from the buccal and the lingual. |
DISCUSSION
Posterior composite resin restorations are now mainstream and represent the majority of posterior intracoronal restorations being placed.11,12 Besides satisfying patient de
sires for natural-looking (nonmetal) restorations, these restorations seal the tooth and provide reinforcement.13-17 However, the placement of composite resin restorations is more demanding for the operator when compared to the placement of amalgam fillings. Many dentists find the multiple steps quite tedious and very time consuming. The concept of “bulk fill” to reduce the time necessary to place and adapt multiple layers of composite resin has been appealing to dentists for some time. In fact, in a “voice of consumer” survey conducted by Kerr, 73% of dentists indicated they would choose a technique for posterior restorations using a bulk-fill, single-shade, and opacity composite resin yielding a possibly identifiable restoration over a material requiring a layering technique with different opacities and shades to achieve imperceptible aesthetics.
 |
 |
| Figure 17. A new, sharp No. 12 blade on a scalpel handle was used to trim any excess. | Figure 18. A 7404 carbide finishing bur (Axis Dental) was used to feather the bonded excess composite beyond the occlusal margins. In the author’s opinion, complete removal of bonded flash is unnecessary and, in fact, it provides additional protection of the margins. |
 |
 |
| Figure 19. Surface finish was achieved with rubber rotary instruments, used wet. | Figure 20. Two-month postoperative view shown wet as the patient sees it. |
 |
 |
| Figure 21. (Second case example.) Preoperative view of failing amalgams. | Figure 22. (Second case example.) Postoperative view at 10 months. |
 |
 |
| Figure 23. Preoperative radiograph of a failing amalgam. |
Figure 24. Postoperative radiograph of the composite resin (SonicFill) restoration. |
 |
 |
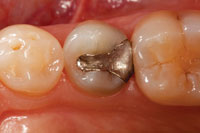
| Figure 25 and 26. Views of the case shown in Figures 23 and 24. The patient requested that the lightest shade (A1) be used and was satisfied with the aesthetics. Postoperative dry view shows matte finish. |
The concern regarding bulk-filled restorations, and the reasons why they haven’t become standard technique, has historically been related to adaptation to cavity walls, depth of cure, and volumetric shrinkage. SonicFill has been optimized to respond to a specific sonic level so the extent of liquefaction upon activation of the handpiece assures intimate adaptation to all cavity walls. Even though this material shows a nice blend of shade and opacity with tooth structure, it still has a 5-mm depth of cure using a high-energy light source. A common perception that a bulk-filled restoration will result in higher shrinkage (leading to higher shrinkage stress) and a poor restoration outcome has not been universally born out by the literature. Although there are published papers which seem to confirm this concern,18 there are several studies contradicting this perception.2,8,19-26 In his paper entitled “Does an Incremental Filling Technique Reduce Polymerization Shrinkage Stresses?” Versluis, et al19 showed that “incremental filling techniques increase deformation of the restored tooth” and concluded that “it is very difficult to prove that incrementalization needs to be retained because of the abatement of shrinkage effects.” In another paper by Idriss, et al21 the conclusion was the “method of placement of a given material had no significant effect on the quality of marginal adaptation.”
| Posterior Resin-Based Composite | ||||||||||||||||||||||||||||||
| Tom M. Limoli, Jr Some of the most commonly performed dental procedures are those identified as direct restorations. All codes in the 2100 and 2300 sequence are considered to be chairside procedures that utilize the direct technique. Direct restorative procedures are those performed directly on a tooth without the use of a die. Third-party payers contractually reimburse only for completed procedures and restorations. They do not reimburse for individual subcomponents or techniques required to complete the procedure. With bonded restorations, the bonding is nothing more than the technique used to complete the procedure. With this combined material and handpiece technique, the procedure would simply be coded as the completed restorative procedure. The additional cost should be reflected in your total fee charged for the restoration. Codes for single and multisurface restorations are not to be used for identifying buildups under crowns. Restorations are identified as replacements of lost tooth structures that involve occlusal and proximal contacts. A restoration must complete the external anatomical outline form of a tooth that is subject to oral bacteria and forces of mastication. Cavity liners and cement bases have no such function and are therefore not separately identifiable as concerns reimbursement. Bases and liners are part of the restoration technique. |
||||||||||||||||||||||||||||||
|
The amount of polymerization shrinkage stress following light curing is the result of many factors, including volumetric shrinkage of the composite itself, polymerization kinetics, modulus of elasticity and the cavity configuration factor (C-Factor), to name a few. Whereas in vitro testing can be a guide (statistical significance), controlled clinical trials have the most relevance (clinical significance). In the absence of such research, which is all too common, the astute clinician is left to rely on what literature does exist, trusted colleagues and teaching clinicians, and his/her own observations. In the 18 months that this author has used SonicFill, the aesthetics have satisfied all patients and the clinical performance has also met the standard of care (Figures 23 and 24). Indeed, the only difference noted has been a significant improvement in placement efficiency and less tedious effort when doing posterior composites.
Another area of concern for some dentists may be patient acceptance of single opacity composite resins from an aesthetic point of view. We are used to seeing photos by teaching clinicians in lectures and in articles where posterior composite restorations often defy detection. As much as we dentists are impressed by this type of beautiful aesthetic posterior dentistry, most patients wonder why we have placed stains in their fillings. The fact is, the vast majority of patients have a different aesthetic standard in the posterior than they do in the anterior (Figures 25 and 26). Yes, they want it tooth-colored and to blend in well, but I believe having the restoration completed faster, at a reasonable fee, would be preferred by all but the most discriminating patient. For those patients who desire imperceptible results, the dentist can place a material that possesses a broader shade range that is also layered with different opacities and the use of tints. Because this takes much more time, an appropriate fee should be charged.
CLOSING COMMENTS
SonicFill clearly breaks from tradition because it uses a single-shade (A1, 2, or 3), single-opacity, fast, 5-mm bulk-fill method of placement without using liners. Significant breakthrough changes such as this can raise skepticism in some clinicians. After all, faster and easier can sometimes be red flags to lower quality. However, in this instance, teeth restored with this composite resin system may have better cavity wall adaptation and less potential for voids. Clinical research on SonicFill is underway in several centers worldwide and early data is very promising. It appears that a material and technology has finally been developed that allows dentists to place posterior composites at an efficiency that rivals amalgam.
References
- Nash R. Patient demand is increasing for posterior aesthetics. Dent Today. 2010;29:74-79.
- Manhart J, Chen HY, Hickel R. Clinical evaluation of the posterior composite Quixfil in class I and II cavities: 4-year follow-up of a randomized controlled trial. J Adhes Dent. 2010;12:237-243.
- Buonocore Memorial Lecture. Review of the clinical survival of direct and indirect restorations in posterior teeth of the permanent dentition. Oper Dent. 2004;29:481-508.
- Daronch M, Rueggeberg FA, De Goes MF. Monomer conversion of pre-heated composite. J Dent Res. 2005;84:663-667.
- Daronch M, Rueggeberg FA, De Goes MF, et al. Polymerization kinetics of pre-heated composite. J Dent Res. 2006;85:38-43.
- Rueggeberg FA, Daronch M, Browning WD, et al. In vivo temperature measurement: tooth preparation and restoration with preheated resin composite. J Esthet Restor Dent. 2010;22:314-322.
- DENTSPLY Caulk. SureFil SDR Flow Technical Product Profile. Clinician Information CD October 2010.
- Braga RR, Ballester RY, Ferracane JL. Factors involved in the development of polymerization shrinkage stress in resin-composites: a systematic review. Dent Mater. 2005;21:962-970.
- Thompson J. Laboratory Research Report: Evaluation of SonicFill Composite. NOVA Southeastern University, October 2010.
- Yapp R, Powers JM. Depth of Cure of Several Composite Restorative Materials. Dent Advis Res Report. 2011;33:1.
- Burke FJ. Amalgam to tooth-coloured materials—implications for clinical practice and dental education: governmental restrictions and amalgam-usage survey results. J Dent. 2004;32:343-350.
- Christensen GJ, Child PL Jr. Has resin-based composite replaced amalgam
? Dent Today. 2010;29:108, 110. - Macpherson LC, Smith BG. Reinforcement of weakened cusps by adhesive restorative materials: an in-vitro study. Br Dent J. 1995;178:341-344.
- Sun YS, Chen YM, Smales RJ, et al. Fracture resistance and microtensile bond strength of maxillary premolars restored with two resin composite inlay systems. Am J Dent. 2008;21:97-100.
- Shor A, Nicholls JI, Phillips KM, et al. Fatigue load of teeth restored with bonded direct composite and indirect ceramic inlays in MOD class II cavity preparations. Int J Prosthodont. 2003;16:64-69.
- Dalpino PH, Francischone CE, Ishikiriama A, et al. Fracture resistance of teeth directly and indirectly restored with composite resin and indirectly restored with ceramic materials. Am J Dent. 2002;15:389-394.
- de Freitas CR, Miranda MI, de Andrade MF, et al. Resistance to maxillary premolar fractures after restoration of class II preparations with resin composite or ceromer. Quintessence Int. 2002;33:589-594.
- Tjan AH, Bergh BH, Lidner C. Effect of various incremental techniques on the marginal adaptation of Class II composite resin restorations. J Prosthet Dent. 1992;67:62-66.
- Versluis A, Douglas WH, Cross M, et al. Does an incremental filling technique reduce polymerization shrinkage stresses? J Dent Res. 1996;75:871-878.
- Neiva IF, de Andrada MA, Baratieri LN. An in vitro study of the effect of restorative technique on marginal leakage in posterior composites. Oper Dent. 1998;23:282-289.
- Idriss S, Habib C, Abduljabbar T, et al. Marginal adaptation of class II resin composite restorations using incremental and bulk placement techniques: an ESEM study. J Oral Rehabil. 2003;30:1000-1007.
- Rees JS, Jagger DC, Williams DR, et al. A reappraisal of the incremental packing technique for light cured composite resins. J Oral Rehabil. 2004;31:81-84.
- Loguercio AD, Reis A, Schroeder M, et al. Polymerization shrinkage: effects of boundary conditions and filling technique of resin composite restorations. J Dent. 2004;32:459-470.
- Loguercio AD, Reis A, Ballester RY. Polymerization shrinkage: effects of constraint and filling technique in composite restorations. Dent Mater. 2004;20:236-243.
- Tachibana K, Kuroe T, Tanino Y, et al. Effects of incremental curing on contraction stresses associated with various resin composite buildups. Quintessence Int. 2004;35:299-306.
- Gallo JR III, Bates ML, Burgess JO. Microleakage and adaptation of Class II packable resin-based composites using incremental or bulk filling techniques. Am J Dent. 2000;13:205-208.
Dr. Jackson practices comprehensive restorative and cosmetic dentistry in Middleburg, Va. He is a 1972 graduate of West Virginia University School of Dentistry. He is an accredited Fellow in the American Academy of Cosmetic Dentistry, a Fellow in the AGD, a Diplomate in the American Board of Aesthetic Dentistry, and is director of the Mastering Dynamic Adhesion and Composite Artistry programs at the Las Vegas Institute for Advanced Dental Studies. He has published many articles on aesthetic, adhesive dentistry and has lectured extensively across the United States and abroad. Dr. Jackson has presented at all the major US scientific conferences as well as to aesthetic academies in Europe, Asia, and South America. He can be reached via e-mail at [email protected].
Disclosure: Dr. Jackson discloses that he acted as a consultant in the development of SonicFill (Kerr) and retains a financial interest in it.


