INTRODUCTION
The most common restorative procedure today is the placement of a direct resin-based composite. As you talk to colleagues, take any continuing education courses, or read any message boards, the reality of placing composites presents real challenges, no matter your level of practice or experience. Preparation depth, secondary caries, adhesion details, and light-curing requirements, as well as the difficulty of re-establishing the contact, consume the conversation. Each of these components has a great influence on the final restorative outcome and should never be underestimated. Ultimately, the practice’s bottom line reflects how you manage the necessary procedural methods and time.
According to the ADA, the most common causes for postoperative sensitivity after placing composite resins are polymerization shrinkage and stress, incomplete material coverage, and under-curing.1 Analyzing this study and its findings a bit closer, technique and material choices are standout concerns that clinicians could improve upon. To ensure success, composite placement requires the understanding of current materials, the manner in which they can be leveraged, and the translation of their benefits into a consistent technique that can create the best long-term outcome for the patient.
This article will outline key components upon which clinicians can build a foundational approach to posterior composite placement. Emphasis will be placed on adhesion detail, utilizing universal bonding agents, bulk-fill composites that offer lower stress chemistries and improved adaptation, and current light-curing science. These “ABC” basics of composite placement will provide improved effectiveness and clinical efficiency.
Adhesion
What is almost invisible, and seems to be the simplest part of a resin restorative procedure, is the selection and application of the adhesive system. The tooth-composite interface is a vital component for ensuring long-term success, but, unfortunately, there seems to be a lot of confusion in the profession regarding bonding agents, such as which generation to use, their benefits, and how they are applied.
Adhesion involves 2 differing substrates—enamel and dentin—that, in turn, must then bond to a restorative material. By removing calcium and phosphate minerals from the enamel surface via etching, a very historical and predictable bond is created.2 However, bonding to dentin is, by just the sheer nature of its organic content, more uncertain.
The most recent bonding agents introduced are termed universal and represent the eighth generation of adhesive materials. Some examples of universal adhesives are All-Bond Universal (BISCO Dental Products), Elect (Dentsply Sirona), One Coat 7 Universal (COLTENE), Scotchbond Universal (3M), Futurabond U (VOCO), OptiBond XTR and OptiBond eXTRa (KaVo Kerr), Universal Bond (Tokuyama Dental America), Clearfil Universal (Kuraray America), and Adhese Universal (Ivoclar Vivadent). These adhesives are filled with chemistry that combines etching, priming, and bonding into one bottle, allowing for an etch mode that best serves the given presenting anatomy. Clinicians are able to customize each direct or indirect restoration by utilizing a selective-etch, total-etch, or self-etch technique.
Current universal bonding agents contain hydroxyethylmethacrylate (HEMA) (a hydrophilic monomer) and water in their formulations. Many include a phosphate ester, such as 10-methacryloyloxydecyl dihydrogen phosphate (10-MDP) as their primary adhesive functional monomer. The addition of 10-MDP offers a hydrophobic component to the adhesive interface as it has been shown to ionically bond to calcium in hydroxyapatite to form stable MDP-Ca salts. Ultimately, post-op sensitivity is minimized. Although these chemistries offer great improvement, by no means should a clinician consider shortcuts in technique or manufacturer recommendations.
Translating the universals’ benefits to the everyday clinician is significant. Adhesion can now be accomplished with one bottle that allows for procedural customization, reduces the number of steps, streamlines inventory, and offers predictable results that are efficient.
Bulk-Fill Resins
A second foundational element that dentists can leverage are bulk-fill resins. From their chemical composition, flowable dental composites volumetrically shrink. Some shrink as little as 3.1%, while others contract near 6.7%. As any resin photo-polymerizes, the material contracts and develops polymerization shrinkage. Polymerization shrinkage is directly related to post-op sensitivity due to the stress (or C-factor) that results from the bonded surfaces vs the free surfaces. This C-factor becomes relevant as the number of bonded surfaces increases, lending more potential for ensuing polymerization stresses to result and impose potential fractures, de-bonding, and/or failure.3
The traditional 2.0-mm incremental composite placement was promoted to further support the stress reduction to limit post-op sensitivity. While this method is certainly very viable, it is operator-sensitive and time-consuming. A myriad of issues can begin to arise clinically, including contamination, voids, isolation, and time to cure, between each added layer.
To offset these events, bulk-fill resins were developed that offer unique chemistry (Venus Bulk Fill [Kulzer], Filtek Bulk Fill [3M], SureFil SDR + [Dentsply Sirona], Estelite Bulk Fill Flow [Tokuyama Dental America], Reveal HD Bulk [BISCO Dental Products], Tetric EvoCeram Bulk Fill [Ivoclar Vivadent], SonicFill [KaVo Kerr], and x-tra fil Fast bulk Fill [VOCO]). Many bulk fills provide much less polymerization shrinkage, flow well in undulating surfaces, can be placed in 4.0- to 5.0-mm increments, and often release fluoride. They also offer varying viscosities. The obvious advantages of these types of materials are improved adaptation, fewer voids due to less manipulation, and reduced placement time. Again, it is best to follow the manufacturer’s directions regarding placement depth, and to not exceed the increment and overfill, which, in turn, creates an under-cured resin material.
Curing
The final consideration of composite placement is light-curing efficiency. Referring back to the study mentioned initially,3 under-curing composite is a common reality, and, when you add bulk-fill composites to the discussion, our clinical confidence in fully curing resin depths is challenged.
Not all curing lights are created equal. To completely ensure adequate resin polymerization, you must utilize a curing light that functions within the wavelength of the material’s photo-initiators. Ideally, today’s curing light emits 1,000 mW/cm2, offers a collimated beam, and provides enough power to allow for a 4.0- to 5.0-mm increment (such as with a bulk fill) to be cured within 20 seconds. The curing light must also possess the proper irradiance, which is essentially the focus of the power on a specific surface utilizing the correct wavelength. Other notable features are the depth-of-cure performance from the light source and the amount of time needed to cure the resin.
Ultimately, operator control of the curing light comes into question. To provide thorough curing, the curing light must be at right angles and as close to the restoration as possible, be stabilized by a finger rest, and produce no shadows that can result from curing. One recently introduced curing light (Bluephase G4 LED [Ivoclar Vivadent]) has an automated assistance system that helps the operator keep the light properly aligned and at the right distance from the composite.
And, as always, you should never decrease the allotted curing time. Shortcutting any method or technique only sets you back.
CASE REPORT
A patient presented with a lower right quadrant in need of restorations: an existing occlusal-buccal amalgam on a first molar with recurrent decay and new decay on the second molar.
The patient was administered a local anesthetic, and the treatment quadrant was isolated with a rubber dam (Figure 1). The decay and amalgam were initially removed using a #330 carbide bur in a high-speed handpiece (Figure 2). Deeper decay was removed at 15,000 rpm with a #6 and #8 CeraBur (Komet). A caries indicator dye further confirmed healthy and unaffected dentin. Because these restorations were both Class I, the author was aware of the importance of not only reducing any potential polymerization stresses by selecting an appropriate bulk-fill resin, but in also choosing and placing a material that could properly adapt to the undulating pulpal floor with the ability to self-level.
 |
 |
| Figure 1. A patient presented with an existing occlusal-buccal amalgam that had recurrent decay on a first molar and a second molar with decay. | Figure 2. The completed restorative preparations, showing decay removal and rounded design. |
 |
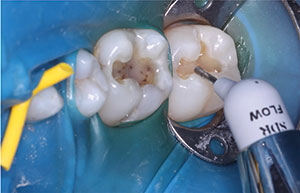 |
| Figure 3. Illustration of a selective-etch technique. | Figure 4. Application and adaptation of bulk-fill flowable composite resin (SureFil SDR [Dentsply Sirona]). |
 |
 |
| Figure 5. Final placement and curing of composite resin. Notice the adaptation and sculpted anatomy. | Figure 6. The final restorations after verifying occlusion, finishing, and polishing. |
Relying on anatomic adhesion principles, a selective-etch technique incorporating a universal bonding agent (Prime&Bond Elect [Dentsply Sirona]) was chosen for both restorations. A 35% phosphoric etch gel was carefully placed on the enamel for 15 seconds (Figure 3). The etch was rinsed thoroughly for 10 seconds, allowing for wet surfaces to remain. The high evacuation suction was tented on each preparation to remove excess water, with the goal being to allow for a moist surface to receive the adhesive agent. The universal bonding agent was freshly dispensed onto a micro-brush that was directly delivered to each preparation and then agitated for 20 seconds per the manufacturer’s directions.
The author chose this particular acetone-based universal bonding agent since it has one of the lowest film thicknesses out of the products on the market. Each preparation received a gentle zig-zag stream of clean, syringed air to thin the bonding agent, starting approximately 0.5 inches above the preparations and nearing the surfaces for 5 seconds. Care was taken to ensure that a shiny surface remained that did not move with the air stream. An LED curing light (Smart Lite Focus [Dentsply Sirona]) was closely positioned over the adhesive surface and held in place for 20 seconds on each restoration.
Next, a unidose bulk-fill resin material (SureFil SDR [Dentsply Sirona]) was syringed into each preparation. Care was taken to keep the tip submerged when placing it, reducing any chance of bubbles or voids and also not violating the 4-mm placement depth. Note the self-leveling property of this flowable bulk-fill (Figure 4). Each placement was light cured from the occlusal surface for 20 seconds.
Finally, a composite capping layer of 2.0 mm was placed using TPH Spectra ST, shade A1 (Dentsply Sirona). This specific material handles well and stays placed, allowing for sculpting anatomy to expedite the finishing process. Each addition was light cured for 20 seconds from both the occlusal surface and the buccal surface (Figure 5). Each restoration was finished using a bullet-style 12-fluted carbide and then finally polished with point and cup Enhance diamond-impregnated polishers, using a light touch that yielded a durable luster. The rubber dam isolation was removed, and the occlusion was verified (Figure 6). The patient was very pleased.
CLOSING COMMENTS
Dental materials have evolved. With that in mind, as clinicians, our restorative choices should shift to maximize each material’s properties. In doing so, we are able to offer not only the best clinical outcome for our patients but also provide procedural efficiency and effectiveness. The end result is a win-win for all those involved.
References
- Sarrett DC. Flowable composites. ADA Professional Product Review. 2009;4:2-13.
- Dudney TE. Universal adhesives. Inside Dentistry. 2017;13:52.
- Ganesh N, Strassler HE. Posterior composite resin restorations: keys to long-term survivability. Compend Contin Educ Dent. 2019;40120-121.
Dr. Trost received her dental degree from the Southern Illinois University School of Dental Medicine. She maintains a private practice in the Greater St. Louis area. Dr. Trost offers postgraduate courses to dentists and their team members that draw from her extensive private practice experience and focus on restorative dentistry, digital technology, dental materials, orthodontics, business management, and patient communication. She is an author, clinical evaluator, and editorial board member and is listed as one of Dentistry Today’s Leaders in Continuing Education. She can be reached at loritrost.com or via email at trost@htc.net.
Disclosure: Dr. Trost reports no disclosures.
Related Articles
Shedding the Right Light on Aesthetics
Evolution and Revolution: Groundbreaking Changes in Composite Dentistry











