INTRODUCTION
The study of occlusion is important to the general practitioner as it relates not only to patient comfort and stability of natural teeth, but also to the longevity of the restorations we place. Before we can evaluate and treat occlusal problems, though, we must first understand what an ideal occlusion looks like. Occlusion for the restorative dentist is commonly understood as having the tempromandibular joint (TMJ) in its most orthopedically stable position as defined by centric relation (CR),1 the masticatory muscles in functional harmony, the teeth intercuspating simultaneously with equal intensity in CR, and anterior guidance in harmony with the envelope of function.2,3 When restoring any of the occluding surfaces with a procedure that requires the use of a laboratory, the transfer of the correct maxillomandibular relationship is critically important in order to reduce occlusal adjustments on the new restoration.
There are several key elements that need to be communicated to the dental laboratory technician to ensure success: preoperative photographs, shade photographs, an accurate full-arch impression of the prepared teeth, a face-bow transfer, a full-arch opposing model, and accurate bite records. The use of a semi-adjustable articulator will more closely replicate the patient’s intraoral condition.4 Provisional restorations should be done correctly in order to protect the pulp, and to provide for positional stability and good occlusal function. Provisional restorations must also be strong, retentive, aesthetic, cleansable, and have excellent marginal integrity. There are numerous provisional materials that can be used with success; however, inattention to this vital step will contribute to, among other problems, shifting of the prepared tooth, which results in an unpredictable fit of the final restoration.5
The purpose of this article is to give the restorative dentist some practical techniques that have been time tested and proven to greatly reduce and eliminate the frustrations of wasted time, compromised results, and a lack of predictability with a particular emphasis on the transfer of accurate interocclusal records to the laboratory.
CASE REPORT
Diagnosis and Treatment Planning
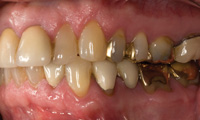
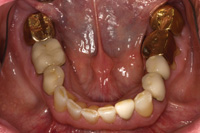
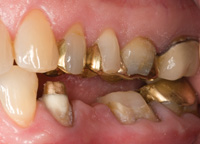
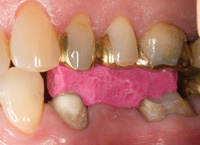
A patient presented with a porcelain-fused-to-gold (PFG) fixed partial denture replacing the lower left second premolar (Figure 1). The bridge had been in place for approximately 30 years. A hole had worn through the occlusal surface of the molar abutment and significant recurrent caries had developed (Figure 2). The bridge also had defective margins. The first premolar had a history of endodontic treatment and was restored with a cast post and core.
 |
 |
|
Figure 1. Defective bridge, teeth Nos. 19 to 21. |
Figure 2. Occlusal decay in perforation of gold abutment on tooth No. 19. |
A thorough exam revealed a stable TMJ, masticatory muscles, and mild periodontitis with scattered 4 mm pockets posteriorly. Many old but serviceable restorations, in addition to the decay previously discussed, were also present. The occlusion had been previously equilibrated so that maximum intercuspation and CR were coincident.
Treatment options were discussed with the patient and he elected to replace the existing restoration with a new bridge. The treatment plan included scaling and root planning the posteriors.
Clinical Treatment Phase
The old bridge was removed, decay removed from the molar and a composite buildup was placed (Filtek Supreme [3M ESPE]). Once the preparations were refined, a double-cord technique (Ultrapack [Ultradent Products]) was used to aid in capturing the margins in a full-arch vinyl polysiloxane (VPS) impression (Affinis [Coltène Whaledent]).
Factors to Consider for Bite Registrations
Before taking a bite record, one must consider that there are 5 criteria for accuracy of an interocclusal bite record as described by Dawson:6
- The bite record must not cause any movement of teeth or displacement of soft tissue.
- It must be possible to verify the accuracy of the interocclusal record in the mouth.
- The bite record must fit the dental casts as accurately as it fits the mouth.
- It must be possible to verify the accuracy of the bite record on the dental casts.
- The bite record must not distort during the storage or transportation to the dental laboratory.
 |
|
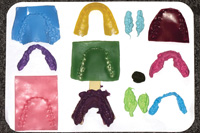
Figure 3. Many bite registration materials are unstable, leading to inaccuracies. |
To fulfill these requirements it is imperative that a stable material be selected for the record. There are many waxes, putties, and pastes that are advertised as bite registration materials. Many of these do not meet the requirements for stability, and if used, will introduce errors in the mounting process and therefore into the final restoration7 (Figure 3). The reality of this situation is that most dental technicians do not use the bite records that they receive; instead, they will hand articulate the casts based on the wear facets of the opposing teeth.
Some of the more common errors can be traced to the use of a flexible VPS material, the use of soft wax, and the techniques employed with these materials. Flexible VPS materials, whether injectible or hand mixed, make it impossible for the dental laboratory technician to verify the exact position of the casts because of springback when the material is compressed, thus allowing a range of possible locations instead of providing pinpoint accuracy. An unknown amount of polymerization (setting) shrinkage and distortion occurs if removed from the mouth before the material reaches its complete set. Certain waxes can also have a memory, and also have the added disadvantage of distortion due to temperature fluctuations in the time between removal from the mouth and arrival at the dental laboratory.
Bite Registration Technique
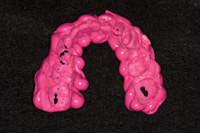
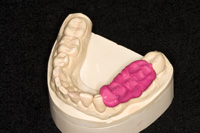
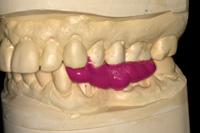
Once the bite registration material has been selected, it is recommended that for quadrant dentistry, the bite record material be trimmed to cover only the prepared teeth and not the entire arch (Figure 4). The VPS material is, in essence, taking an impression of the occlusal surfaces of both arches as the patient closes into the desired interocclusal position (either CR or maximum intercuspal position [MIP]). If the master model and the opposing model do not have the same level of accuracy, the record will not fit (Figures 5 and 6). Because of the perforations where the teeth contact, the record is extremely thin, flexible, and will many times tear or break in handling.
 |
|
Figure 4. Untrimmed excess material introduces mounting errors. |
 |
 |
|
Figures 5 and 6. Even if a quadrant section is used, the untrimmed excess makes it impossible to verify the accuracy of the mounting. |
Finally, the same level of care should be taken to record the opposing arch as well as the preparations; distortion in the impression will lead to a distorted model that will not fit the bite record, no matter what technique you use. Always measure the water and powder if using a standard alginate impression material for the opposing arch. The use of full-arch metal nonperforated rimlock trays (DENTSPLY Caulk) will provide a consistent and accurate method since the alginate material will not pull out of the tray on removal from the mouth.
 |
 |
|
Figure 7. The preparations. |
Figure 8. Rigid bite registration, properly trimmed to view tooth-bite record-tooth with no voids. |
 |
 |
|
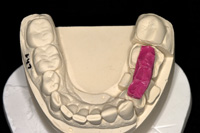
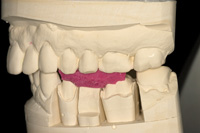
Figure 9. Occlusal view of a properly trimmed bite record. |
Figure 10. Transfer of bite record to the model for accurate mounting and easy verification by the dentist and dental technician. |
The dental stone selected to pour these impressions should have an expansion of no more than 0.08% and be measured carefully and vacuum mixed. The use of a stable material and proper technique will help both the dental technician and the clinician achieve predictable results. In this case, because there was no discrepancy between CR and MIP, it was possible to record the bite with the patient fully occluded in CR/MIP, transferring the vertical dimension of occlusion along with the interarch relationship. Use of a more rigid injectable bite registration (such as Futar D [Kettenbach]) can accomplish the goals of an accurate bite record as long as it is trimmed to fit just over the occlusal surfaces of the preparations, and just inside the buccal cusp of the opposing cusps. The clinician should be able to see tooth-bite registration-tooth intraorally with absolutely no spaces in between, and no rocking (Figures 7 and 8). This trimming and verification step gives the doctor and the dental technician confidence that the mounting should look exactly the same (Figures 9 and 10). If there is any discrepancy, the dentist and dental technician should discuss any possible sources of error. Open communication between the dentist and the dental technician is critical for resolution of many potential problems.8,9
Open Bite Records Verses Semi-Adjustable Articulators
 |
 |
|
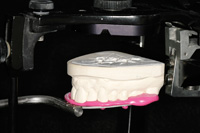
Figure 11. Face-bow registration with material covering full arch. |
Figure 12. Upper model fits accurately into the bite registration with no rocking. |
It is important to note that when using an open bite record technique that a face-bow transfer and the use of a semi-adjustable articulator are mandatory or mounting errors will increase. The use of the same rigid bite registration material on the bite fork will eliminate the inherent errors in wax, which has been traditionally used. It is recommended to cover the entire bite fork with the material, as opposed to small dots of material in various locations around the arch. This seemingly small detail will ensure that the dental technician has only one positive location that the upper cast will fit into thus contributing to the accuracy of the mounting. Excess should be trimmed away so that only the cusp tips engage the cast to be sure the laboratory technician can visualize whether or not the model is completely seated (Figures 11 and 12).
Laboratory Procedures
 |
 |
|
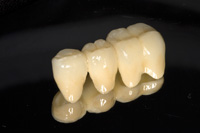
Figure 13. Finished porcelain-fused-to-zirconia bridge. |
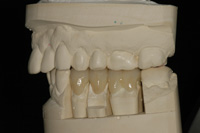
Figure 14. Fit was verified on the model. |
When the mounting is complete and the dies are separated and trimmed, the fabrication process begins. A second pour of the master impression is used to create a solid model to check interproximal contacts. In this case, porcelain-fused-to-zirconia was chosen to replace the previous PFG bridge. The zirconia framework was fabricated utilizing CAD/CAM technology (Vericore [Whip Mix]) (Figure 13). Layering porcelain was applied (GC Initial ZR-FS and GC Initial IQ luster paste [GC America]), contoured and adjusted to fit the opposing model (Figure 14).
Seating Appointment
 |
 |
|
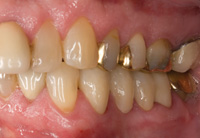
Figure 15. Exceptional marginal fit was observed. |
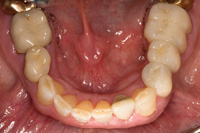
Figure 16. Very minimal adjustment was required at delivery. |
Upon try-in the marginal fit of the new bridge was excellent10 and no interproximal adjustment was needed. The restoration was inserted using a self-etching, self-adhesive resin ce-ment system (RelyX Unicem [3M ESPE]). Only minimal occlusal adjustment was done. The patient was pleased with the result, and with good oral hygiene, looks forward to many years of service from the new restoration (Figures 15 and 16).
CONCLUSION
The process of predictable treatment begins with a complete examination protocol and continues through excellent communication with the dental laboratory technicians. This process culminates with an excellent outcome that will give the patient long-term comfort, function, health, and maintainability.
In the restorative process, accurate bite records have long been a concern of dental technicians. The use of a more rigid material, which has been trimmed properly for use in quadrant dentistry, will aid the dental technicians in the mounting process and fabrication of any restoration. Given enough occlusal and axial reduction, a skilled dental technician can produce extremely aesthetic restorations that require minimal adjustment. This will not only preserve the artistry incorporated into the new work, but will also decrease the time needed for delivery while increasing patient satisfaction and confidence in the dentist and team.
Acknowledgement
The author would like to express his gratitude to Rick Sonntag, RDT (4 Points Dental Designs, St. Petersburg, Fla) for the fabrication of the restoration in this case report.
References
- The glossary of prosthodontic terms. J Prosthet Dent. 2005;94:10-92.
- Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St Louis, Mo: Mosby; 1989.
- Okeson JP. Management of Temporomandibular Disorders and Occlusion. 6th ed. St. Louis, Mo: Mosby Elsevier; 2008.
- Adams DC. Articulators: should we accept the status quo? A doctor-technician liaison’s perspective. Dent Today. 2006;25:56, 58-59.
- Shillingburg HT Jr, Hobo S, Whitsett LD, et al. Fundamentals of Fixed Prosthodontics. 3rd ed. Chicago, Ill: Quintessence Publishing; 1997.
- Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, Mo: Mosby; 2007.
- McKee JR. Comparing condylar position repeatability for standardized versus nonstandardized methods of achieving centric relation. J Prosthet Dent. 1997;77:280-284.
- Vasquez D, Vasquez B. Partnering for success. Doctor/technician communication. Dent Today. 2003;22:112-114,116-117.
- Small BW. Laboratory communication for restorative excellence. Gen Dent. 2006;54:86-87.
- Sonntag R. First Look-Versus CAD/CAM. J Dent Tech. 2008;25(4).
Dr. Scott attended the University of Kentucky College of Dentistry and completed a General Practice Residency at the Medical College of Georgia School of Dentistry. He maintained a private restorative practice in Ft. Myers, Fla, before becoming a partner at the International Center for Complete Dentistry with Glenn DuPont, Witt Wilkerson, Ken Grundset, and Kim Daxon in St. Petersburg, Fla. Dr. Scott lectures nationally on restorative and cosmetic dentistry and implementing complete dentistry into private practice. He is a member of the American Academy of Restorative Dentistry, American Academy of Cosmetic Dentistry, American Dental Association, and the Florida Dental Association. He is also a Fellow in the Inter-national College of Dentists and is a faculty member of the Dawson Academy in St. Petersburg. He can be reached at (727) 821-4433 or jscott@icfcd.com.
Disclosure: Dr. Scott reports no conflicts of interest.